News
Online decision aid addresses health disparities among MSM
(April 2017) An online tool promoting shared decision making about HIV-prevention among men who have sex with men (MSM) is being evaluated in two clinical settings--Beth Israel Deaconess Medical Center and Fenway Health. HCC worked with Douglas Krakower, MD, the study’s principal investigator, to develop UP: Understanding PrEP, a decision tool for men and their healthcare providers. (Because it is part of ongoing research, right now it is accessible only by login by study participants.)
The HCC team named the decision aid, developed its content and visual approach, and built and programmed the tool.
A promising option but barriers exist
 The majority of new HIV infections in the US occur in MSM. Pre-exposure prophylaxis with a daily pill is more than 90% effective in preventing HIV transmission for this priority population. However, limited knowledge about PrEP among MSM and primary care physicians, and potential misconceptions about this promising intervention, are barriers that may limit its impact in clinical settings.
The majority of new HIV infections in the US occur in MSM. Pre-exposure prophylaxis with a daily pill is more than 90% effective in preventing HIV transmission for this priority population. However, limited knowledge about PrEP among MSM and primary care physicians, and potential misconceptions about this promising intervention, are barriers that may limit its impact in clinical settings.
The purpose of the decision aid is to help healthcare providers and MSM make informed, collaborative decisions about PrEP by increasing their knowledge and facilitating their engagement in brief, goal-oriented discussions about whether PrEP is an appropriate option.
UP was developed through an iterative process using the Ottawa Decision Support Framework (ODSF). Qualitative interviews assessed how MSM and providers weigh the risks and benefits of PrEP use and decide whether to initiate PrEP. Prototypes were tested and refined before HCC began developing the online tool.
Four steps to an informed decision
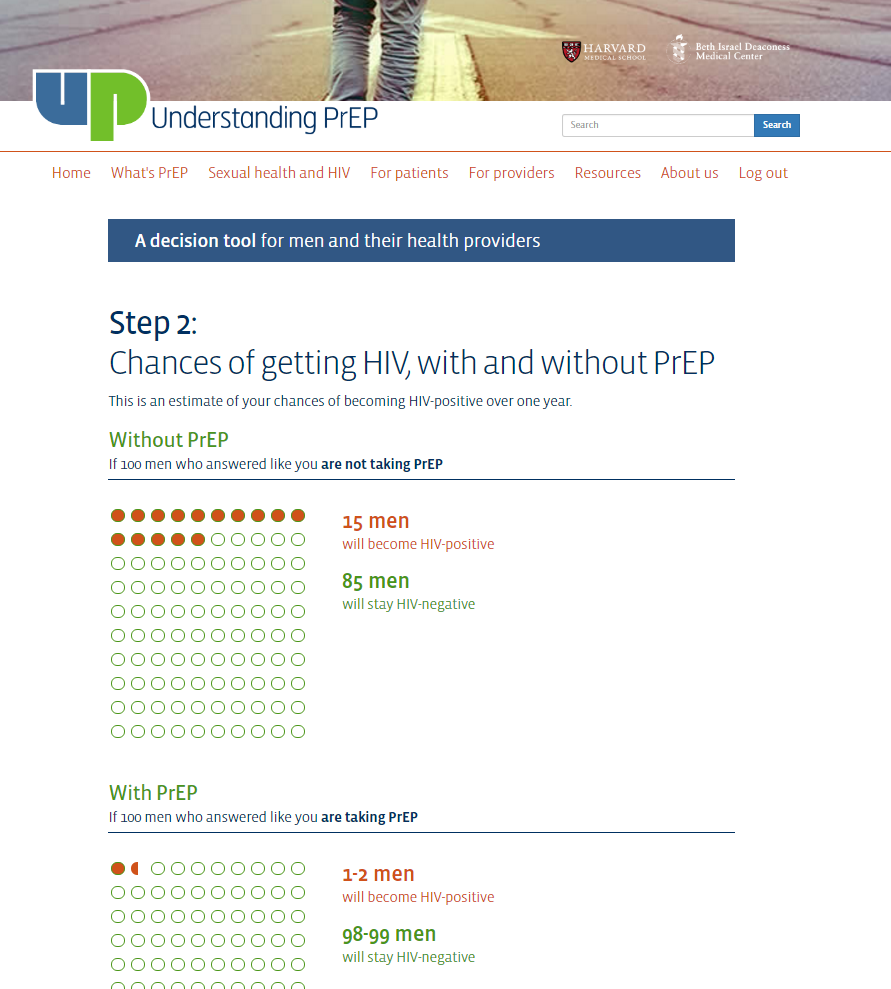
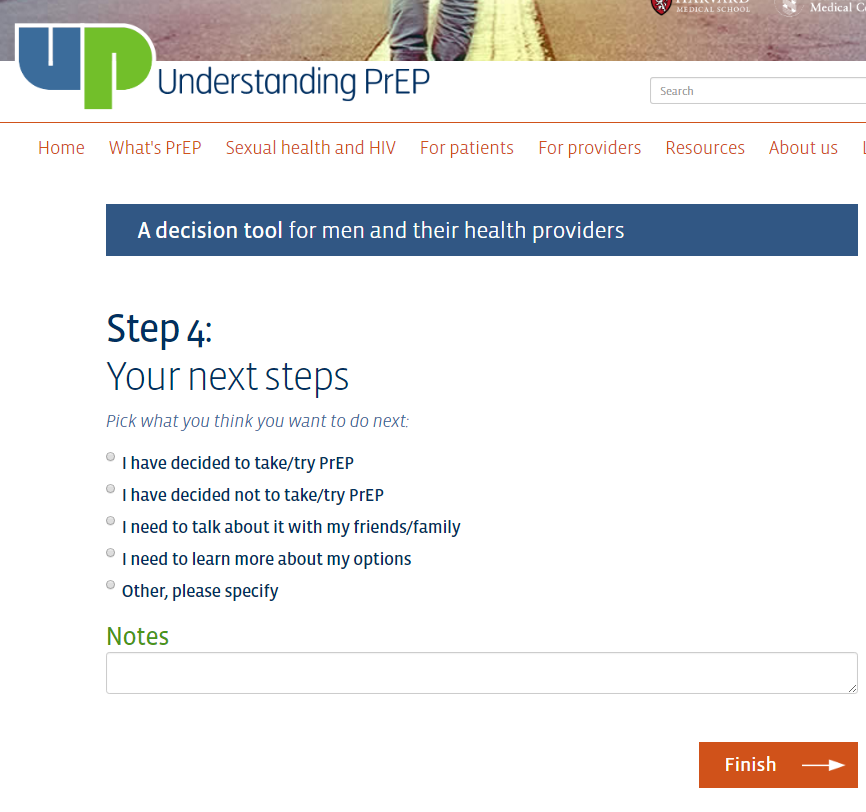 The decision aid integrates a decision-support tool for patients and a risk-prediction tool for providers. Users complete four steps--a brief survey of personal risk behaviors, a visual display of an individual’s estimated risk of acquiring HIV and the potential benefits of PrEP, interactive exercises to clarify personal values and preferences about using PrEP, and identification of an actionable next step. Notes can be added while progressing thru the steps, and a downloadable summary report can be printed at the end. To protect confidentiality, no data are stored on the website.
The decision aid integrates a decision-support tool for patients and a risk-prediction tool for providers. Users complete four steps--a brief survey of personal risk behaviors, a visual display of an individual’s estimated risk of acquiring HIV and the potential benefits of PrEP, interactive exercises to clarify personal values and preferences about using PrEP, and identification of an actionable next step. Notes can be added while progressing thru the steps, and a downloadable summary report can be printed at the end. To protect confidentiality, no data are stored on the website.
The tool can be completed by a patient in advance of a clinical visit, or initiated by the provider during a visit. Because men and providers may not always be fully comfortable talking about sexual health, supplemental content for patients offers guidance on how to initiate a discussion about PrEP with their providers, and a provider-facing section includes prescribing information, suggestions for incorporating the decision aid into clinical care, and additional resources (e.g., links to normative guidelines).
Communicating cultural relevance
Studies have found that many MSM, given the disproportionately high rates of new HIV infections in this community, have concerns about acquiring HIV that may negatively impact their sexual health and well-being. The benefit of reducing their worries about HIV while having sex was identified by participants in focus groups as a significant motivation for considering PrEP. HCC incorporated images that convey personal connection and intimacy to engage users and highlight the relevance of the tool to the intended audience.
The site’s visual approach also helps affirm the trustworthiness of the tool, a key concern for MSM who may use the tool and providers alike.
Next steps
After the current study is completed, Dr. Krakower’s goal is to test UP more broadly in a larger study and/or to make this tool accessible for public use. Although several online PrEP decision aids currently exist, UP has the advantage of having been developed using a rigorous, evidence-based process. So far, public health leaders and LGBTQ advocates have been enthusiastic about this project, its completion, and its eventual dissemination for use online and in clinical settings.
